- 65 Mario Capecchi Drive, Salt Lake City, Utah,84132
- 175N 400W, #C10, Orem, Utah,84057
- 2255N 1700W, Layton, Utah,84041
- 617 E. Riverside Drive, St. George, Utah,84790
- 552 N. Dixie Drive, St. George, Utah,84770
- Harley Street, London, ,W1G8
- 1025 E. 3300 S., Suite B, Salt Lake City, Utah,84106
Treatment of Obstruction
Traditional Surgical Treatments
Since its introduction in the early years of this century, Incisional dacryocystorhinostomy (DCR) has been the "traditional" procedure most often relied upon for relief of epiphora (chronic tearing) and nasolacrimal duct obstruction in adults. However, the high success rate (> 90%) for incisional DCR is balanced by a number of potential drawbacks:
-
Recovery time is significant
-
An incisional scar might possibly develop due to invasive procedure
-
Potential for excess bleeding
-
May not be necessary for partial obstructions
-
goal: anastomosis between lacrimal sac and nasal cavity (middle meatus)
-
decreased success with prior nasal fractures, children, nasal mucosal disease, broad flat nasal bridge, and re-operation
-
AnesthesiaIncision
-
General
- because of pt anxiety during bony excision
-
MAC with Local
- with 2% lidocaine/epinephrine with deep infiltration to bone
- pack middle turbinate of nose with nasal neosynephrine/Afrin/Cocaine mixture
-
General
-
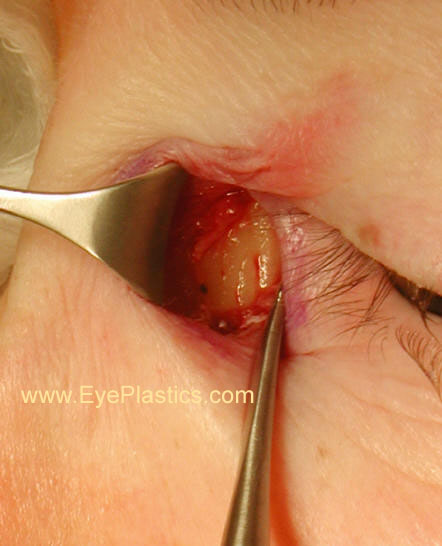
- avoid angular vessels, prevent bowstring contractures causing epicanthal folds
- dissect skin from muscle with Tenzel periosteal elevators
- spread orbicularis off periosteum with Steven’s or elevators just lateral to medial canthal tendon (push to bone, then spread)
- vertically incise periosteum 2 mm medial to ant lacrimal crest, dissect away posteriorly, lacrimal sac reflected (supero)temporally
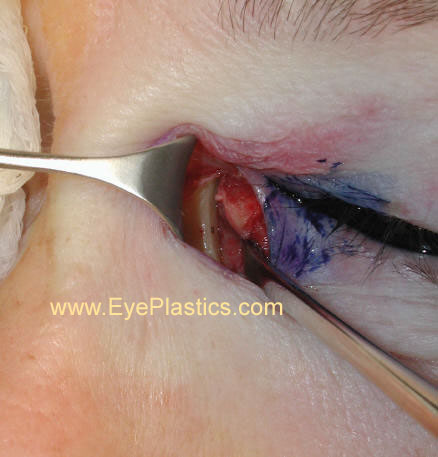
- with hemostat, elevators, or drill, fracture posterior to ant lac crest through lac bone/sac fossa
- kerrison ronjeurs to make opening; be sure to get superior enough (under medial canthal Tendon); smooth edges
- inject local into nasal mucosa to blanch tissue and dissect from bone with muscle hook(27 g 1.5 in needle)
- incise mucosa over intranasal cotton swab with blade, make sure ant flap is large enough; often no post flap
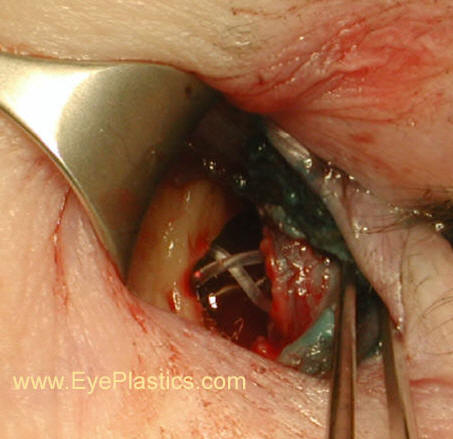
- probe both canaliculi
- cut into sac over probe, be sure to be completely through sac (might possibly need to pass wescotts to make sure); make sure you have enough anteriorly
- /- relaxing incisions in flaps
- suture posteromedial flap of lacrimal sac to posterolateral lip of incised nasal mucosa if possible using 4-0 double arm chromic or 5-0 dexon
- intubate and tie silastic tubes together at level of nasal osteomy with 6-0 nylon/silk to prevent prolapse into eye
- optional: bring balloon end of cut (red rubber catheter) Foley catheter tube though nose then though ostium, fill balloon then pack it back just inside nose to stent apart tissues, provide post-op hemostasis, to be removed early post-op
- suture anterolateral sac flap to anteromedial nasal mucosal lip using 2-prong hook for exposure
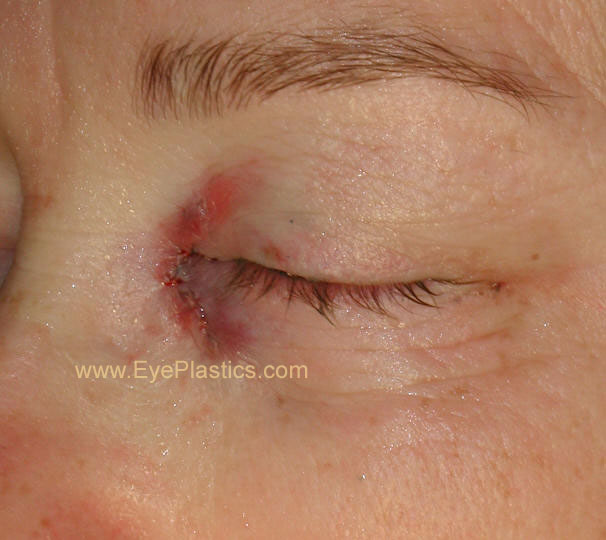
- close deep tissue with vicryl, then skin with suture of choice
- tie ends of tubes together with multiple throws, suture to lateral vestibule
|
 |
 |
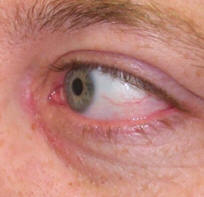 |
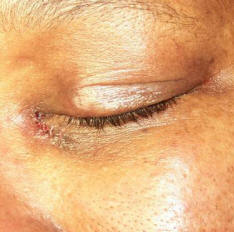
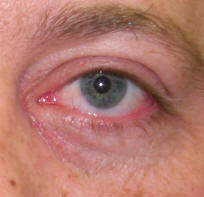
| 3 weeks after left DCR, incision is barely noticeable | |
|
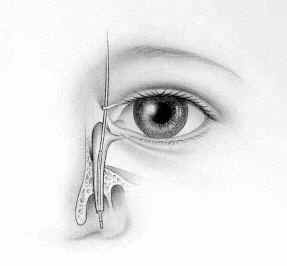
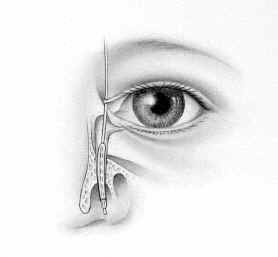
STEP 1:
The LacriCATH ® balloon catheter (shown in the picture) is inserted through an opening in the corner of the eye and down into the tear duct .® balloon catheter (shown in the picture) is inserted through an opening in the corner of the eye and down into the tear duct .balloon catheter (shown in the picture) is inserted through an opening in the corner of the eye and down into the tear duct . |
 |
|
STEP 2:
The balloon catheter is inflated with sterile water to dilate the tear duct for a period of 90 seconds. It is then deflated, and reinflated for 60 seconds. |
 |
|
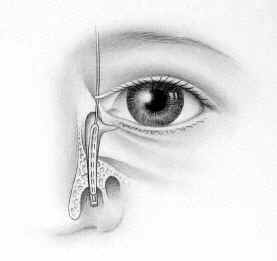
STEP 3:
The balloon catheter is then repositioned slightly higher in the duct and inflated twice as in step 2. |
 |
The balloon catheter is then deflated and removed.
 |
 |
|
Here you can see the balloon as it is inflated within the nose
|
|
Movies of Surgical Lacrimal Duct Procedures
Lacrimal Stents
CDCR / JONES tube / PG tube
If the "tear duct" obstruction is beyond repair, It might possibly be necessary to surgically implant an artificial "tear duct" behind the inner corner of the eyelids to drain the tears into the nose. The artificial "tear duct" is made of Pyrex glass and is called a "Jones tube." or Putterman-Gladstone (PG) tube.

These might possibly be purchased at Gunther Weiss Glass Science, located in Portland Oregon. 503-644-3507
Dacryocystorhinostomy surgery provides relief to millions of people every year who suffer from tear duct problems ranging from collapsed tear ducts and excessive tearing caused by accident or injury, birth defects or environmental strain. Left untreated, patients might possibly experience swelling, infections, increased swelling, tearing ("wet eye") and severe pain.
In 1961, Lester T. Jones and Gunther Weiss paired up to develop a solution for tear duct problems. They developed highly specialized glass tubes (called "Lester T. Jones Tear Duct Tubes") designed for insertion into the nasolacrimal duct. The body develops scar tissue around the tube, which holds it in place, forming a new permanent tear duct.
Gunther Weiss Scientific Glass Blowing Company offers Lester T. Jones Tear Duct Tubes in a variety of lengths and diameters to address most patient needs. In adds to, tubes can be custom-fabricated to accommodate unique angles and sizes

